Rectus sheath
Dr Richard Craig
Content
- Indications
Specific contraindications
Anatomy
Technique
Volume of LA
Specific complications
Self-Assessment
Bibliography
Indications
A rectus sheath block provides intraoperative and postoperative analgesia for mid-line abdominal incisions. Specifically, it may be useful for the following operations:
- Umbilical hernia repair
- Paraumbilical hernia repair
- Epigastric hernia repair
- Pyloromyotomy
- Laparoscopic surgery
- Abdominoplasty
- Excision of urachal remnants
- Duodenal atresia repair
Rectus sheath catheters have been used for upper abdominal surgery (1). The rectus sheath block has also been used for chronic pain management for patients with abdominal cutaneous nerve entrapment, myofascial pain syndrome, and iatrogenic nerve injury. (2)
Specific contraindications
Local infection
Anatomy
- The skin of the anterior abdominal wall is supplied by the ventral rami of the inferior six thoracic nerves. These are the continuation of the T7 to T11 intercostal nerves and the subcostal nerve (T12). The anterior cutaneous branch of the ventral rami passes through the posterior of the rectus sheath. The rectus abdominis muscle originates from the pubic symphysis and pubic crest, and inserts into the xiphoid process and 5th to 7th costal cartilages. It is innervated by the ventral rami of the inferior six thoracic nerves.
- The two rectus muscles are separated by the linea alba. The lateral border of the rectus muscle and its sheath form the linea semilunaris.
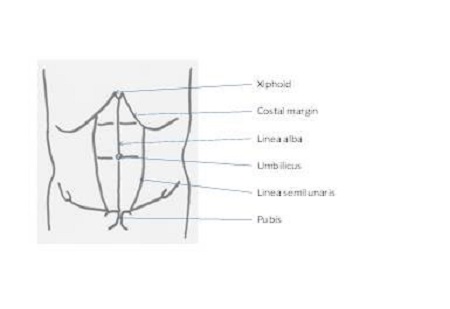
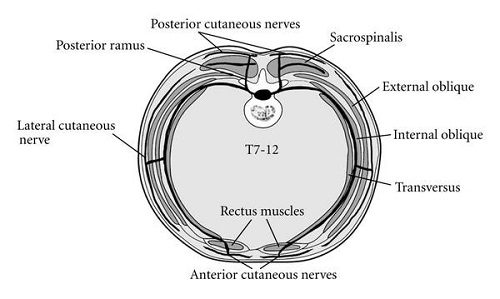
- The rectus sheath encloses the rectus abdominis muscles and is formed by the aponeuroses of the three flat abdominal muscles; the external oblique, internal oblique and the transversus abdominis muscles. The external oblique aponeurosis and the anterior layer of the internal oblique aponeurosis form the anterior wall of the rectus sheath. The transversus abdominis aponeurosis and the posterior layer of the internal oblique aponeurosis form the posterior wall of the sheath. The fibres of the anterior and posterior walls of the sheath interlace in the mid-line to form the linea alba.
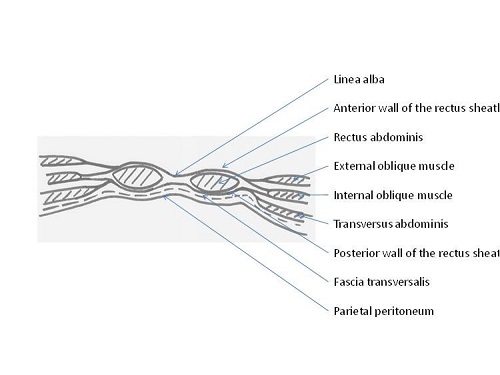
- The inferior quarter of the posterior wall of the rectus sheath is deficient; the arcuate line forms the inferior border of the posterior wall of the rectus sheath. The arcuate line is midway between the umbilicus and the pubic crest.
- The anterior layer of the rectus sheath is firmly attached to the rectus abdominis muscle at three tendinous intersections. These are usually located at the level of the xiphoid process, the umbilicus and half-way in between. The tendinous intersections do not extend through the whole rectus abdominis muscle to the posterior sheath; It is because of this local anaesthetic can spread caudad and cephalad in the plane between the rectus muscle and the posterior rectus sheath.
- The superior and inferior epigastric vessels and the terminal parts of the inferior five intercostal and subcostal vessels and nerves are located within the rectus sheath. The inferior epigastric artery is a branch of the external iliac artery. It runs superiorly in the transversalis fascia to enter the rectus sheath at the arcuate line. The superior epigastric artery is a branch of the internal thoracic artery (internal mammary artery) and it enters the rectus sheath just inferior to the 7th costal cartilage.
US technique
- The patient is placed supine.
- Ensure yourself and the ultrasound machine are placed ergonomically.
- Select the estimated ultrasound depth. In neonates this will usually be 2cm, infants 3cm, thereafter 4cm depth is usually an appropriate starting scanning depth.
- A linear probe is placed transverse on the abdomen, just above the umbilicus.
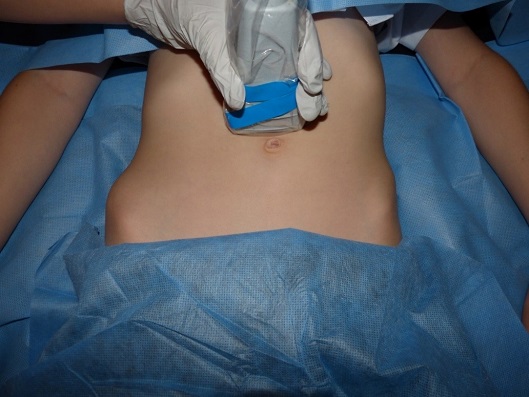
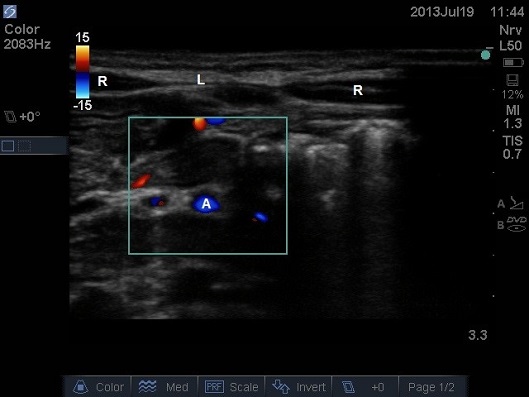
ULTRASOUND OF NEONATAL ABDOMEN IN TRANSVERSE PLANE. A – AORTA, L – LINEA ALBA, R – RECTUS MUSCLE
- Select highest appropriate frequency for the initial scanning depth.
- The initial image will have the linea alba in the midline with a rectus abdominis muscle either side.
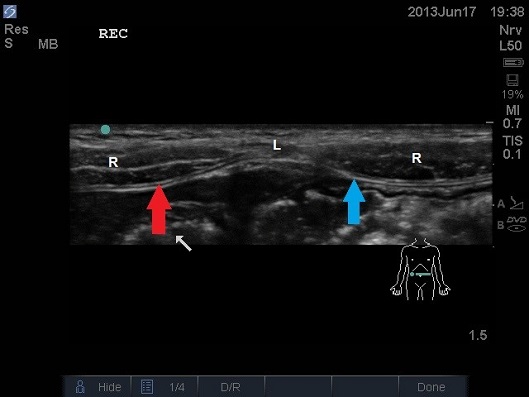
ULTRASOUND OF INFANT ABDOMEN IN TRANSVERSE PLANE. WHITE ARROW – BOWEL, BLUE ARROW FASCIA TRANSVERSALIS AND PERITONEUM, RED ARROW POSTERIOR FASCIA,L – LINEA ALBA, R – RECTUS MUSCLE.
- Move the probe laterally and scan the rectus abdominis muscle in the transverse plane. As the probe is moved laterally the semilunaris (lateral border) is visualised.

- Just lateral to the semilunaris the 3 lateral muscles are seen to come together.
- Note in neonates the muscle will only be a couple of millimetres thick.
- In larger children it is possible to identify the epigastric vessels with Doppler. Ensure the probe pressure is minimal.
- Deep to the rectus sheath is a continuous hyperechoic line that is the peritoneum, it crosses the midline.
- Insert the block needle in-plane, the puncture point should be suitably lateral that the needle will have a shallow trajectory.
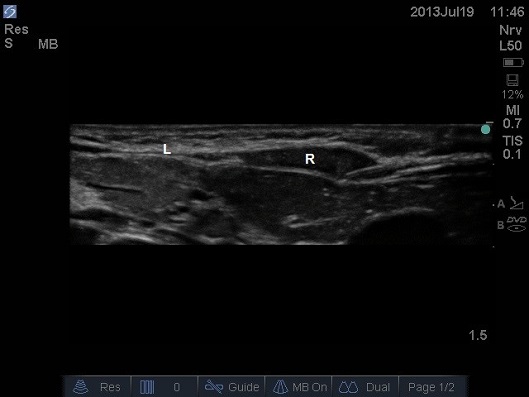
ULTRASOUND OF NEONATAL ABDOMEN IN TRANSVERSE PLANE. NEEDLE HAS A SHALLOW TRAJECTORY COMING FROM LATERAL TO MEDIAL, AND THE BEVEL IS UPPERMOST. THE ANTERIOR SHEATH IS TENTED. THIS CHILD HAS HEPATOMEGALY SECONDARY TO HEART FAILURE, NOTE THE LIVER DIRECTLY BENEATH THE RECTUS MUSCLE. L – LINEA ALBA (MIDLINE), R – RECTUS MUSCLE (NOTE HOW THIN THE MUSCLE IS IN THE NEONATE, APPROXIMATELY 2MM THICK)
- Note it can be difficult to puncture the skin, either lift the skin and push the needle through or make a knick in the skin using a sharp bevelled needle.
- Aim to position the tip of the needle between the rectus abdominis muscle and the posterior rectus sheath.
- Stop the needle tip just superficial to the first white line (the posterior sheath) as a ‘pop’ is not felt or seen in all patients.
- Aspirate and inject 0.25-0.5mls, if the tip is in the correct plane the muscle is peeled off the posterior sheath. If the needle tip remains too superficial then an intramuscular injection occurs; then the needle is carefully advanced.
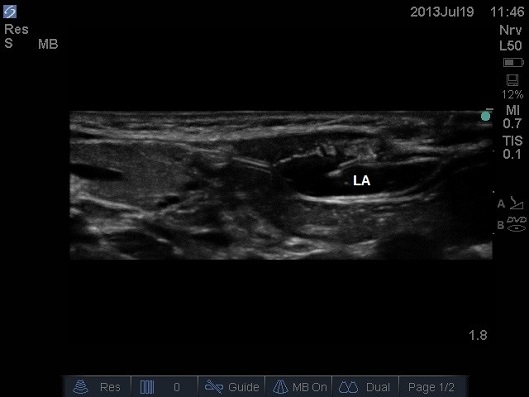
ULTRASOUND OF NEONATAL ABDOMEN IN THRANSVERSE PLANE. THE LOCAL ANAESTHETIC (LA) PEELS THE POSTERIOR SHEATH OFF THE RECTUS MUSCLE.
- The tissues are often quite tough even in a neonate; therefore a steady pressure may be required.
- A ‘pop’ is not always present and it may be necessary to repeat the test injection of local anaesthetic.
- In neonates prevent waste of precious local anaesthetic by using saline to detect the correct plane.
- Deposit local anaesthetic in the potential space between the rectus abdominis muscle and the posterior aspect of the sheath.
- After injection spread can be assessed by turning the probe in the paramedian longitudinal plane, local anaesthetic will be seen to spread beneath the tendinous intersections.
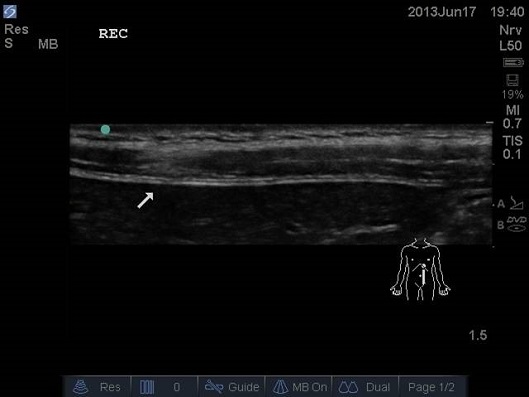
ULTRASOUND OF NEONATAL ABDOMEN IN PARAMEDIAN LONGITUDINAL PLANE. WHITE ARROW – SEMIRENTNDINOUS INTERSECTION (NOTE THAT IT IS NOT FIRMLY ATTACHED POSTERIORLY).
(Insert still ultrasound images and video of block.)
Volume of LA
- A volume of 0.1 ml/kg/side of 0.25% levobupivacaine has been shown to be adequate for umbilical hernia repair (3).
- For neonates 0.125% levobupivacaine is effective.
- A larger volume will potentially spread from the xiphoid to the pubis; Up to a total of 0.8 ml/kg 0.25% levobupivacaine may be used.
- The absorption kinetics of ropivacaine are slower after a rectus sheath block than after other compartment blocks (4).
Specific complications
- Peritoneal puncture
- Perforation of the bowel
- Visceral puncture
- Major vessel puncture
- Mesenteric vessel puncture
- Inferior epigastric vessel puncture
- Retroperitoneal haematoma.
Top tips
- Ensure a shallow trajectory
- Not every patient has a ‘pop’ on entering the correct plane
- In neonates use 0.125% levobupivacaine
Self-assessment questions
Bibliography
- Comish P, Deacon A. Rectus sheath catheters for continuous analgesia after upper abdominal surgery. ANZ Journal of Surgery. 2007. Vol. 77, p. 84.
- Skinner AV, Lauder GR. Rectus sheath block: successful use in the chronic pain managment of pediatric abdominal wall pain. Paediatric Anaesthesia. 2007. Vol. 17, 12, pp. 1203-11.
- Willschke H, Bosenberg A, Marhofer P, Johnston S, Kettner SC, Wanzel O, Kapral S. Ultrasonography-guided rectus sheath block in paediatric anaesthesia – a new approach to an old technique. British Journal of Anaesthesia. 2006. Vol. 97, 2, pp. 244-9.
- Wada M, Kitayama M, Hashimoto H, Kudo T, Kudo M, Takada N, Hirota K. Brief reports: plasma ropicacaine concentrations after ultrasound guided rectus sheath block in patients undergoing lower abdominal surgery. Anesthesia & Analgesia. 2012. Vol. 114, 1, pp. 230-2.
